National Back Awareness
Low Back Pain
Back Pain Explained
– best viewed on desktop PC
Back pain treatment in Wimbledon
Contrary to popular belief back pain is less connected with sitting posture 1 than previously thought. More significant is the correlation with psychological distress2 which doubles the chances of developing low backpain. However back pain straddles mechanical and emotional boundaries which can make its management difficult, if not dealt with promptly.
Latest NICE guidelines3 recognise a combination of advice, exercise, manual therapy and psychological therapy are the most effective in managing low back pain. Since 1986, the Living Centre Clinic has brought all these together in one single treatment programme to help thousands of patients with acute and chronic low back pain.
Low back pain at a deeper level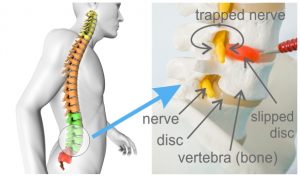
Pain from the spine arises in 2 ways. i) from the tissue damage itself, which surprisingly causes the milder symptoms; and the body's response to the damage, which causes the majority of a patient's symptoms. The picture shows the delicate disc and nerves (the ligaments are not shown). If these are threatened the body produces powerful muscle spasms, along with large amounts inflammatory fluid. This is the reason why doctors prescribe muscle relaxants and anti-inflammatory drugs. It's great at treating the symptoms, but it does not necessarily address the underlying tissue damage.
Top Tips for Beating Low Back Pain
1. Acute Back Pain
 Hot or Cold? Until proven otherwise, ice is best. Even if your muscles are in spasm, something must be underneath causing that to happen. Spasms are a sign something has strained or torn, so muscle do the only thing they can do – tighten up – to protect the injury. Heat does remove a spasm, but that could make it worse as the body loses it's protection. Of course to reduce the spasm by a small amount is helpful. However please note that conversely heat increases inflammation (& ice and ibuprofen remove it). Be care careful not to work one against the other.
Hot or Cold? Until proven otherwise, ice is best. Even if your muscles are in spasm, something must be underneath causing that to happen. Spasms are a sign something has strained or torn, so muscle do the only thing they can do – tighten up – to protect the injury. Heat does remove a spasm, but that could make it worse as the body loses it's protection. Of course to reduce the spasm by a small amount is helpful. However please note that conversely heat increases inflammation (& ice and ibuprofen remove it). Be care careful not to work one against the other.

Movement or Stillness? In the very early moments of the attack it makes sense to follow the body's lead which usually works to ‘freeze' an area. This means within the first day or two, being still is best. The most common error is to sit still in a chair or on a PC. So avoid all forms of sitting initially, we suggest only sit for your meals and to use the bathroom. Ideally, you could try lying down interspersed with movement, ie walking in your home.
 Sleep & Sleeping. Healing is most active during your night's sleep. So each hour before midnight is worth two hours after midnight. So try a week of early nights, ie by 10pm latest. Avoid sleeping on your stomach or on the side which hurts. Generally its best to sleep on the side which does not hurt, possibly with a pillow between the knees. You may also sleep on your back, possibly with a pillow or two under the knees.
Sleep & Sleeping. Healing is most active during your night's sleep. So each hour before midnight is worth two hours after midnight. So try a week of early nights, ie by 10pm latest. Avoid sleeping on your stomach or on the side which hurts. Generally its best to sleep on the side which does not hurt, possibly with a pillow between the knees. You may also sleep on your back, possibly with a pillow or two under the knees.
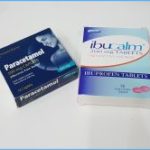 Paracetamol vs Ibuprofen. The best medication is ibuprofen (Neurofen). This is an anti-inflammatory medicine and will help dry the damage area fast. This is important because your body cant lay down healing fibres if the area is still wet – the fibres wont bond. Ice (cold packs) and ibuprofen work together in the same way. You can try natural alternatives such as Turmeric and Devil's Claw remedies as well. Paracetamol however is a painkiller and will only mask the symptoms.
Paracetamol vs Ibuprofen. The best medication is ibuprofen (Neurofen). This is an anti-inflammatory medicine and will help dry the damage area fast. This is important because your body cant lay down healing fibres if the area is still wet – the fibres wont bond. Ice (cold packs) and ibuprofen work together in the same way. You can try natural alternatives such as Turmeric and Devil's Claw remedies as well. Paracetamol however is a painkiller and will only mask the symptoms.
2. On Going Back Pain
- Neutral spine postition: lie on the floor with your knees bent or supported on a chair at 90° with a pillow under your head
- Continue with your normal activities BUT take your time and DON’T push yourself
- Before getting up bring your knees to your chest one at a time
- Bend your knees when bending over or picking up objects off the floor
- When carrying objects keep it close to your body
- Avoid sitting for long periods – keep getting up
 Tips to get you out of your chair
Tips to get you out of your chair
- Set your phone or PC to beep every 30-45 minutes.
- Drink more water, so you will have to go to get up more often to move about.
- If you work in a high-rise building use the stairs to go the rest room on another floor.
- Get out of your chair to speak to a colleague (rather than email them).
- Consider using a standing desk, or at least rest raise your monitor and keyboard higher if possible.
Home Massage Tips
Knowing where to massage and how much to do it for is key. Generally resist the temptation to massage the injured tissue. Medical evidence4 shows that areas which are painful are not actually “stiff”, “jammed” or “locked”, despite the feeling that it is. It is typically more effective to massage the same area on ‘other' side of the spine; and/or the area above or below the injury. This is because these tissues will be compensating and would benefit from a little rest. This in turn will help them support the injury, so aiding nature cure.
Note: please be aware in acute cases of pain, no matter how tempting to rub an injured tissue, rubbing may make it worse. It may create more tissue damage, increase inflammation, or result in more muscle spasm. We always recommend massaging away from the site of injury.
How to get out of bed / Pick up something from the floor
Free Exercise PDF (including videos)
 Jennifer Beck M.OST
Jennifer Beck M.OST
Osteopath
Female Wellness
Call 0208 946 2331 to see how we we can help you today.
NOTE: all advice and exercises are for guidance only. Every pain is different. These exercises may not agree with every back-pain complaint, so please stop immediately if pain arises. You are adviced to seek professional help before following the advice or exercises.
References
- Korshoj, M., Hallman, D., Mathiassen, S. E. & Asdahl, M. Is objectively measured sitting at work associated with low back pain? A cross sectional study in the DPhacto cohort. Is objectively measured sitting at work associated with low back pain? A cross sectional study in the DPhacto cohort (2017). Available at: http://www.diva-portal.org/smash/record.jsf?pid=diva2%3A1109002&dswid=9585. (Accessed: 25th September 2017)
- Power, C., Frank, J., Hertzman, C., Schierhout, G. & Li, L. Predictors of low back pain onset in a prospective British study. Am. J. Public Health 91, 1671–1678 (2001).
- Nice.org.uk. NICE Guidline, Low back pain and sciatica in over 16s: assessment and management. https://www.nice.org.uk/guidance/ng59/resources/low-back-pain-and-sciatica-in-over-16s-assessment-and-management-pdf-1837521693637. ISBN: 978-1-4731-2186-7. (2016).
- Stanton, T. R., Moseley, G. L., Wong, A. Y. L. & Kawchuk, G. N. Feeling stiffness in the back: a protective perceptual inference in chronic back pain. Sci. Rep. 7, (2017).